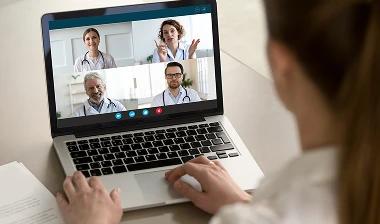
Study locates five genes that may play a critical role in Lewy body dementia.
Source: National Institutes of Health
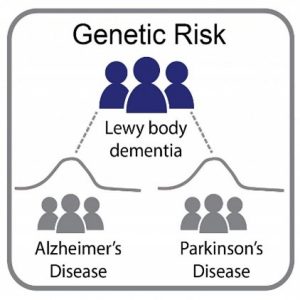 An NIH-led genetic study found that Lewy body patients had higher chances of suffering Alzheimer’s or Parkinson’s disease than age-matched controls. Credit: Scholz lab NIH/NINDS.Scholz lab NIH/NINDS
An NIH-led genetic study found that Lewy body patients had higher chances of suffering Alzheimer’s or Parkinson’s disease than age-matched controls. Credit: Scholz lab NIH/NINDS.Scholz lab NIH/NINDS
In a study led by National Institutes of Health researchers, scientists found that five genes may play a critical role in determining whether a person will develop Lewy body dementia. The results supported the disease’s known ties to Parkinson’s disease and also suggested that people who have Lewy body dementia may share similar genetic profiles to those who have Alzheimer’s disease.
Most cases are considered ‘sporadic’, meaning there is no known genetic role; one theory is that the risk for developing LBD is driven by a combination of genetics and environmental factors. A growing body of evidence suggests genetics may play a role in LBD and that some cases may be inherited.
About the Study
Researchers compared the chromosomal DNA sequences of 2,981 people with LBD with those of 4,931 healthy, age-matched control participants. Initially, they found that the sequences of five genes from the people with LBD were often different from those of the controls. This suggested that these genes may be important.
It was the first time that two of the genes, called BIN1 and TMEM175, had been implicated in the disease. These genes may also have ties to Alzheimer’s and Parkinson’s diseases. The other three genes, SNCA, APOE, and GBA, had been implicated in previous studies, and thus, strengthened the importance of the genes in Lewy body dementia. The researchers were able to confirm these results by comparing the DNA sequences of another 970 people with LBD with a new set of 8,928 control subjects.
Further analysis suggested that changes in the activity of these genes may lead to dementia and that the GBA gene may have a particularly strong influence on the disease. The gene encodes instructions for beta-glucosylceramidase, a protein that helps a cell’s recycling system break down sugary fats. The researchers found that both common and rare variants in the GBA gene are tied to Lewy body dementia.
Comparing Genetic Risks with Alzheimer’s and Parkinson’s
Next, the researchers analyzed data from previous studies on Alzheimer’s and Parkinson’s disease. They found that the genetic profiles of the participants in this study had higher chances of suffering from either Alzheimer’s or Parkinson’s disease than the age-matched control subjects. These predictions held even after they lowered the potential impact of known Alzheimer’s and Parkinson’s disease-causing genes, like APOE and SNCA. Interestingly, the patient’s genetic risk profiles for Alzheimer’s disease, on the one hand, or Parkinson’s disease, on the other, did not overlap.
The senior author of the study, Sonja Scholz, MD, Ph.D., is an investigator at the NIH’s National Institute of Neurological Disorders and Stroke (NINDS) and a member of LBDA’s Scientific Advisory Council. “Although Alzheimer’s and Parkinson’s disease are molecularly and clinically very different disorders, our results support the idea that the problems that cause those diseases may also happen in Lewy body dementia,” said Dr. Scholz. “The challenge we face in treating these patients is determining which specific problems are causing the dementia. We hope studies like this one will help doctors find precise treatments for each patient’s condition.”
New Research Resource
To help with this effort, the team published the genome sequence data from the study on the database of Genotypes and Phenotypes (dbGaP), a National Library of Medicine website that researchers can freely search for new insights into the causes of Lewy body dementia and other disorders.
Reference: Chia, R., et al. Genome sequencing analysis identifies new loci associated with Lewy body dementia and provides insights into the complex genetic architecture. Nature Genetics, February 15, 2021 DOI: 10.1038/s41588-021-00785-3